Understanding and treating PD
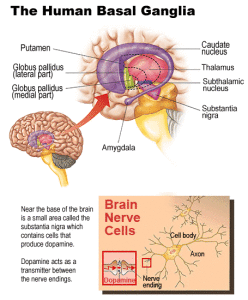
PD was never really understood until 1960. An Austrian team lead by Oleh Hornykiewicz performed autopsies on human PD patients at the University of Vienna. The knowledge at this point – established by autopsy – was that this very specific, human illness, was caused by a very specific part of the human brain degenerating. The substantia nigra, part of the brain found in the basal ganglia was badly affected. This was never likely to be uncovered in animals, who don’t have a comparable basal ganglion. As an expert explains, animal models “do not reflect the complexities of the human basal ganglion.”[4]
The Austrian team discovered that the nigostriatial pathway had degenerated and had very little dopamine. Dopamine regulates movement and emotion, and normally carries most of the nerve signal.
This made perfect sense as PD does affect movement and emotion, and led to tests on brain tissue from PD patients, which confirmed the dopamine deficiency. They went on to discover that nerves containing dopamine die, leaving a deficiency of dopamine. They soon gave patients treatment intended to lead to dopamine production, which caused immediate benefits. As well as revolutionising PD treatment, this enabled better research into other neurological illnesses including epilepsy and schizophrenia. As one expert put it, Hornykiewicz had “fundamentally changed how neuropharmacology is practiced.”[5]
Hornykiewicz was never awarded the Nobel Prize for this work, although it was awarded to a team who had followed on from the work pioneered by the Austrians. The award attracted disapproval: 250 neurologists criticised the decision and the decision not to reward Hornykiewicz.[6]
This massive discovery is only a step on the way to finding a cure for this terrible disease. The fact that the substantia nigra dies is a symptom, not the cause of the disease, and further knowledge of why it dies needs to be uncovered. For this reason why need more studies into human patients on a detailed level studying the interactions between the substantia nigra and the rest of the body. Autopsies are now possible on a highly detailed level thanks to improvements in microscope technology, and arguably provide the most valuable of any single method in studying nerological illness.
Two pathologists wrote “In recent years, participants in meetings of the American Association of Neuropathologists have heard criticism about the increasing use of animal models to study human neurologic disease…. A strong cadre of diagnostic and research neuropathologists believe that only human material can provide relevant answers to many problems about human central nervous system disease. In fact, examination of the data bears out this contention. Of the 185 abstracts presented at the 1985 meeting of the American Association of Neuropathologists, 115 (62%) were presentations of human neuropathology, and an astounding 81 (43%) were based on investigations of human brains at autopsy. Among these autopsy studies were seven presentations of either the first complete description of a newly recognized human disorder, or one of the first complete descriptions of an uncommon human neurologic disease.”[7]
Nevertheless, the Austrian discovery made a difference to human patients, as it immediately enabled treatments to enhance dopamine levels. Further human studies showed that Levodopa could be used to stimulate dopamine levels.[8] This is imperfect and becomes less effective over time – the reason for which is understood thanks to study of patients. [9] Another method has been to use the nightshade plant, which decreases levels of acetylcholine, which increases when dopamine is in short supply.
Other effects have been discovered by accident – such as the effect of ecstasy or the antiviral Amantadine.
Before the Hornykiewicz discovery, surgery was used to control PD by removing both thalami. The thalamus is a two part brain section. This had limited success, but it was in attempting these that a more striking method was discovered.